What causes atrial fibrillation?
|
Most common causes |
Less common causes |
- Hypertension (high blood pressure)
- Coronary artery disease
- Heart valve disease
- After heart surgery
- Chronic lung disease
- Heart failure
- Cardiomyopathy
- Congenital heart disease
- Pulmonary embolism
|
- Hyperthyroidism
- Pericarditis
- Viral infection
|
In at least ten percent of the cases, no underlying heart disease is found. In these cases, AF may be related to alcohol or excessive caffeine use, stress, certain drugs, electrolyte or metabolic imbalances, or severe infections. In some cases, no cause can be found.
The risk of AF increases with age, particularly after age 60
How is atrial fibrillation diagnosed?
The most commonly used tools to diagnose atrial fibrillation include:
These monitoring devices help the doctor learn if you are having irregular heart beats, what kind they are, how long they last, as well as what may cause them.
What are the dangers of atrial fibrillation?
Many people live for years with atrial fibrillation without problems. However, chronic atrial fibrillation can result in future problems:
- Because the atria are beating rapidly and irregularly, blood does not flow through them as quickly. This makes the blood more likely to clot. If the clot is pumped out of the heart, it can travel to the brain, resulting in a stroke. People with atrial fibrillation are five to seven times more likely to have a stroke than the general population. Clots can also travel to other parts of the body (kidneys, heart, intestines), causing damage.
- Atrial fibrillation can decrease the heart's pumping ability by as much as 20 to 25 percent. Atrial fibrillation, combined with a fast heart rate over a long period of time, can result in heart failure.
- Chronic atrial fibrillation is associated with an increased risk of death.
What are the symptoms of atrial fibrillation?
You may have atrial fibrillation without having any symptoms at all. If you have symptoms, they may include:
- Heart palpitations - Sudden pounding, fluttering or racing sensation in the chest
- Lack of energy or feeling over-tired
- Dizziness - Feeling lightheaded or faint
- Chest discomfort - Pain, pressure, or discomfort in the chest
- Shortness of breath - Having difficulty breathing during normal activities or even at rest
How is atrial fibrillation treated?
The goals of treatment for atrial fibrillation include regaining a normal heart rhythm (sinus rhythm), controlling the heart rate, preventing blood clots and reducing the risk of stroke.
Many options are available to treat atrial fibrillation. These include medications, lifestyle changes, procedures and surgery. The choice of treatment for you is based on your heart rhythm and symptoms.
Medications
Initially, medications are used to treat atrial fibrillation. The medications may include:
- Rhythm control medications (antiarrhythmic drugs)
These medications help return the heart to its normal sinus rhythm or maintain normal sinus rhythm. There are several types of rhythm control medications, including: Quinidex (quinidine); Pronestyl (procainamide); Norpace (disopyramine); Toprol, Lopressor (metoprolol); Tambocor (flecainide acetate); Rythmol (propafenone); Betapace (sotalol); Tikosyn (dofetilide) and Cordarone (amiodarone).
You may have to stay in the hospital when you first start taking these medications so your heart rhythm and response to the medication can be carefully monitored. These medications are effective 30 to 60 percent of the time, but may lose their effectiveness over time. You may need to try several medications so your doctor can find the best one for you.
Some rhythm control medications may actually cause more arrhythmias, so it is important to discuss your symptoms and any changes in your condition with your doctor.
- Rate control medications (to slow the heart rate)
Rate control medications, such as Lanoxin (digoxin), beta-blockers (example: metoprolol) and calcium channel blockers (example: verapamil, diltiazem), are used to help slow the heart rate during atrial fibrillation. These medications do not control the heart rhythm. 
- Medications to prevent blood clots and reduce the risk of stroke
Anticoagulant or antiplatelet therapy medications, such as Coumadin (warfarin), Xarelto, Pradaxa and Eliquis reduce the risk of blood clots and stroke. Although anticoagulant or antiplatelet drugs reduce the risk of stroke, they do not eliminate the risk. Regular blood tests are required when taking Coumadin to evaluate the effectiveness of the drug. With the other anticoagulants there is no need for blood testing or dietary restrictions.
Some people may be treated with aspirin instead of anticoagulants. Talk to your doctor about the anticoagulant medication that is right for you.
Lifestyle changes
In addition to taking medications, there are some changes you can make to improve your heart health.
- If you notice your irregular heart rhythm occurs more often with certain activities, you should avoid them.
- Quit smoking.
- Limit your intake of alcohol. Moderation is the key. Ask your doctor for specific alcohol guidelines.
- Limit or stop using caffeine. Some people are sensitive to caffeine and may notice more symptoms when using caffeinated products (such as tea, coffee, colas and some over-the-counter medications).
- Beware of stimulants used in cough and cold medications. Some of these types of medications contain ingredients that promote irregular heart rhythms. Read the label and ask your doctor or pharmacist what type of cold medication is best for you.
Procedures
When medications do not work to correct or control AF, or when medications are not tolerated, a procedure may be necessary, such as: electrical cardioversion, catheter ablation, pulmonary vein isolation, ablation of the AV node, or device therapy.
- Electrical Cardioversion: If medications are not able to control a persistent irregular heart rhythm (such as AF), cardioversion may be required. Cardioversion frequently restores a normal rhythm, although its effect may not be permanent. After a short-acting anesthesia is given, an electrical shock is delivered to your chest wall to synchronize the heartbeat and restore a normal rhythm.
- Catheter ablation: Catheter ablation therapy is an option for people who cannot tolerate medications or when medications fail to maintain a normal heart rhythm.
Two types of ablation can be performed including pulmonary vein antrum isolation or ablation of the AV node. Both are performed by an electrophysiologist (doctor who specializes in treating heart rhythm conditions). 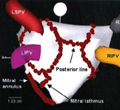
- Pulmonary Vein Isolation: Research has shown that almost all atrial fibrillation signals come from the four pulmonary veins. During this procedure, special catheters are inserted into the heart. Two catheters are inserted into the right atrium and two into the left atrium. The left atrium is accessed through a transeptal puncture.
Intracardiac echocardiogram is used to visualize the left atrium during the procedure. One catheter in the left atrium is used to map or locate the abnormal impulses coming from the pulmonary veins. The other catheter is used to deliver the radiofrequency energy to ablate, or create lesions outside the pulmonary veins. The procedure is repeated for all four pulmonary veins.
The lesions heal and within 4 to 8 weeks, form a circular scar around the pulmonary veins. The scar blocks any impulses firing from within the pulmonary veins, thereby "disconnecting" the pathway of the abnormal rhythm and curing atrial fibrillation.
Ablation of the Av node: During an ablation, catheters are inserted through the veins (usually in the groin) and guided to the heart. Radiofrequency energy is delivered through the catheter to sever or injure the AV node. The end result is a permanent, very slow heart rate because the electrical impulses from the top chamber of the heart cannot travel down to the lower chamber. Therefore, the patient needs a permanent pacemaker to maintain an adequate, sufficient heart rate. This procedure improves atrial fibrillation symptoms, but does not cure the condition. An anticoagulant medication is prescribed to reduce the risk of stroke. Important note: Due to better treatment alternatives, AV node ablation is rarely used to treat atrial fibrillation.
Implantable atrial defibrillator: a device used to treat AF symptoms. When the symptoms of AF occur, the person can turn on the device and treat the AF when appropriate and convenient. Or, the device can be set to operate automatically. The atrial defibrillator can be programmed to identify when a person is having an episode of atrial fibrillation. When it occurs, the device delivers low-dose therapy to convert AF to a normal heart rhythm. This procedure improves atrial fibrillation symptoms, but does not cure the condition.
Permanent Pacemaker : A pacemaker is a device that sends small electrical impulses to the heart muscle to maintain a suitable heart rate. Pacemakers are implanted in people with AF who have a slow heart rate. The pacemaker has a pulse generator (that houses the battery and a tiny computer) and leads (wires) that send impulses from the pulse generator to the heart muscle, as well as sense the heart's electrical activity.
Newer pacemakers have many sophisticated features, designed to help with the management of arrhythmias and to optimize heart rate-related function as much as possible.
Surgical treatment
Patients with chronic AF not relieved by medication or procedures, or patients who have other conditions requiring heart surgery, are candidates for surgical treatment of atrial fibrillation.
During the Maze procedure, a series of precise incisions are made in the right and left atria to confine the electrical impulses to defined pathways to reach the AV node.
Surgical Pulmonary vein isolation is a modification of the Maze procedure in which the surgeon uses alternative energy sources instead of incisions to create lesions. The alternative energy sources used during surgical pulmonary vein isolation include: radiofrequency, cryothermy, microwave and laser. The goal of all four energy sources is to produce lesions and ultimately scar tissue to block the abnormal electrical impulses from being conducted through the heart and promote the normal conduction of impulses through the proper pathway.
Many of these approaches can be performed with minimally invasive (endoscopic or "keyhole") surgical techniques.
Radiofrequency Ablation: A special radiofrequency energy catheter is used to heat the tissue and produce lesions on the heart similar to the lesions of the Maze procedure. There are a variety of surgical techniques related to the type of catheter used, the dose of energy, and the types of lesions created.
Cryotherapy: (also called cryoablation) Very cold temperatures are transmitted through a probe (called a cryoprobe) to create lesions. This technique is used commonly during arrhythmia surgery to replace the incisions made during the Cox Maze procedure.
Microwave Technology: A special wand-like catheter is used to direct microwave energy to create several lesions on the heart. The lesions block the conduction of abnormal electrical beats and restore a normal heartbeat.
Laser: Lasers rapidly create the lesions or lines of conduction block. Laser technology offers promise for the development of additional minimally invasive approaches.
Some patients may have atrial fibrillation in addition to other heart problems (such as valve or coronary artery disease), which require surgery. In these cases, the surgeon may combine the surgical treatment for atrial fibrillation with other surgical therapies to correct the atrial fibrillation and the coexisting heart condition.















